June 19, 2020
Uncovering the Long-term Neurological Ramifications of COVID-19
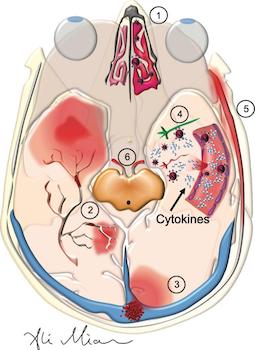
The COVID-19 virus targets the brain in ways that are just now starting to be understood. Patients with COVID-19 can present with a wide range of neurological manifestations that can be due to the injury to central and peripheral nervous system via a cytokine storm, blood clots, direct damage by SARS-CoV-2, and/or molecular mimicry. Apollo Health’s Chief Neuroimaging Science Advisor, Dr. Cyrus Raji, has written a review of what is currently known about this virus and the related clinical neurology which represents the foundation of what will eventually become a separate active field of research.
Dr. Raji says that it’s very important for those who’ve suffered from COVID-19 to focus on optimizing brain health by following the strategies outlined in the Bredesen Protocol to both prevent and remediate any long term damage to the brain and to protect against memory loss. You can see the abstract to his review below and link to full text of the paper here.
Neurobiology of COVID-19 Abstract
Anosmia, stroke, paralysis, cranial nerve deficits, encephalopathy, delirium, meningitis, and seizures are some of the neurological complications in patients with coronavirus disease-19 (COVID-19) which is caused by acute respiratory syndrome coronavirus 2 (SARS-CoV-2). There remains a challenge to determine the extent to which neurological abnormalities in COVID-19 are caused by SARS-CoV-2 itself, the exaggerated cytokine response it triggers, and/or the resulting hypercoagulapathy and formation of blood clots in blood vessels throughout the body and the brain. In this article, we review the reports that address neurological manifestations in patients with COVID-19, who may present with acute neurological symptoms (e.g., stroke), even without typical respiratory symptoms such as fever, cough, or shortness of breath. Next, we discuss the different neurobiological processes and mechanisms that may underlie the link between SARS-CoV-2 and COVID-19 in the brain, cranial nerves, peripheral nerves, and muscles. Finally, we propose a basic “NeuroCovid” classification scheme that integrates these concepts and highlights some of the short-term challenges for the practice of neurology today and the long-term sequalae of COVID-19 such as depression, OCD, insomnia, cognitive decline, accelerated aging, Parkinson’s disease, or Alzheimer’s disease in the future. In doing so, we intend to provide a basis from which to build on future hypotheses and investigations regarding SARS-CoV-2 and the nervous system.




